Contents
Introduction to the QPP and MIPS
The Quality Payment Program (QPP) is a federally mandated Medicare program by Centers for Medicare and Medicaid Services (CMS) that seeks to improve patient care and outcomes while managing the costs of services patients receive.
Clinicians may participate in the Quality Payment Program through one of three reporting options:
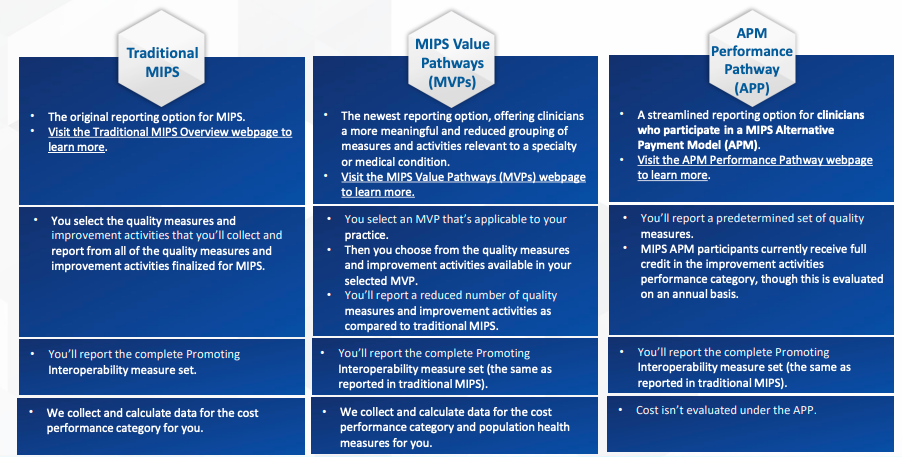
Traditional Merit-based Incentive Payment System (MIPS) is the primary way to participate in the Quality Payment Program. Advanced Alternative Payment Models (APMs) are optional programs that offer different incentive structures for high quality, cost efficient care. An example of participating in the APP is if your practice has signed up to work with an ACO, ACO’s are considered APMs and submit data through the APP.
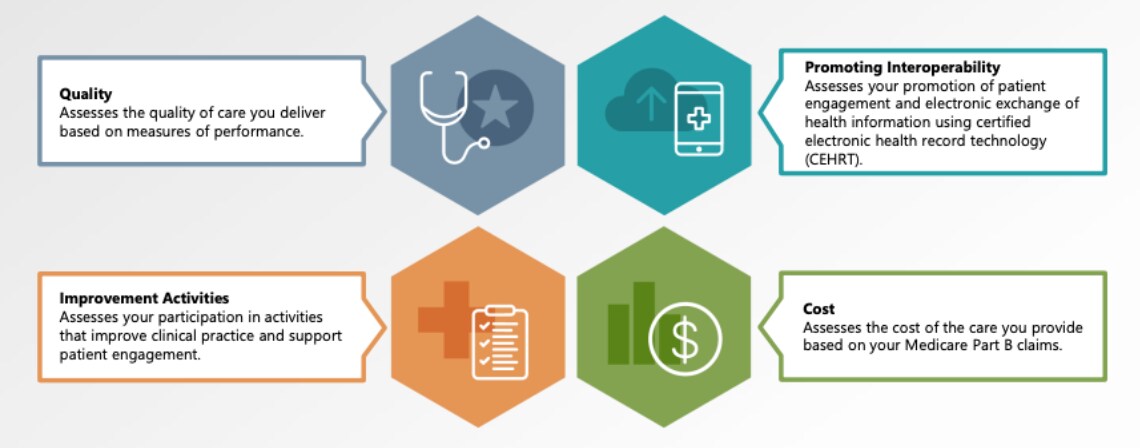
MIPS is the standard fee-for-service (FFS) payment track that applies to around 95% of physicians. Under MIPS, CMS evaluates performance across four categories: Quality, Cost, Improvement Activities, and Promoting Interoperability. Here is a brief description of each category from CMS:
2026 MIPS Eligibility
The following Clinician Types are eligible for MIPS:
- Physicians (MD, DO, DDS, DMD, DPM, OD)
- Osteopathic practitioners
- Chiropractors
- Physician assistants
- Nurse practitioners
- Clinical Nurse Specialists
- Certified nurse anesthetists
- Physical therapists
- Occupational therapists
- Clinical psychologists
- Qualified speech-language pathologists
- Qualified audiologists
- Registered dietitians or nutrition professionals
- Clinical social workers
- Certified nurse-midwives
If any of the following apply to the provider, they are not required to participate in MIPS:
- Fewer than 200 Medicare fee-for-service patients
- Less than $90,000 in Medicare charges
- Fewer than 200 Medicare fee schedule services
- Participate in an Advanced APM
- First-year Medicare provider
Use the CMS’s Participation Lookup website to confirm eligibility.
Interpreting Eligibility
Once you look up your NPI on the CMS Participation Lookup website, locate the “Associated Practice” that is using Elation. You will see one of three possible outcomes. Only one of these outcomes (outline below in orange) requires you to participate in MIPS.

ℹ️ ELIGIBILITY NOTE
If you or your practice are associated with and participating in an APM (ACO or other APM type) contact the APM administrator to determine best practices for MIPS participation and data submission. MIPS APM participation may differ from traditional MIPS participation. MIPS quality data are generally submitted via the APM - an important distinction to understand.
MIPS Performance Categories
Each of the four performance evaluation categories has different requirements that need to be met and each practice’s goal is to maximize points earned. This year, CMS has weighted the categories as follows and is identical to the weights from the 2025 performance year:
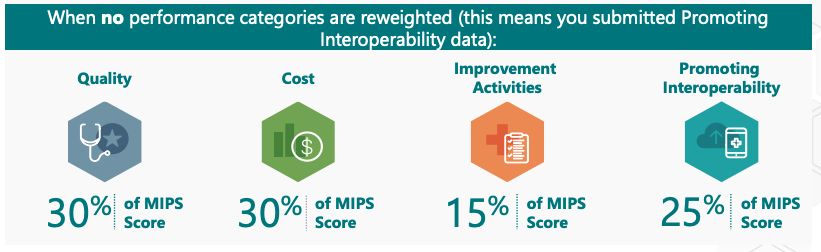
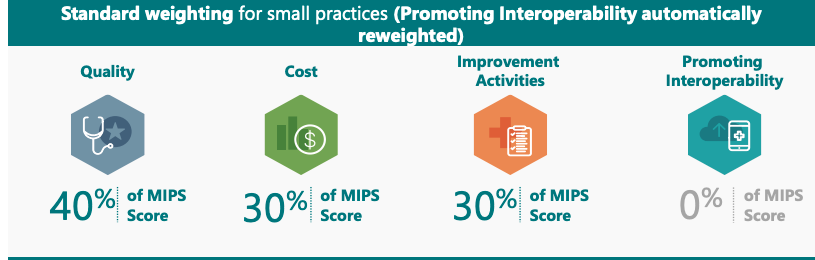
Quality (30%)
One of the highest weighted categories is Quality, which looks at Clinical Quality Measures.
Practices submitting via Traditional MIPS can submit as many measures as they want but are scored on their 6 top-performing quality measures. Data needs to be collected for these measures across at least 75% of their visits. Elation has 12 electronic clinical quality measures (eCQMs)that are used in MIPS that we can report on and with a set of videos that cover workflows. You can also learn more about all the electronic Clinical Quality Measures that Elation supports in the Clinical Quality Measures Reports Guide.
ℹ️ NOTEOne (1) of the 6 measures must be an outcome measure. The outcome measures available in Elation are:
Each measure is scored out of 10 points. The provider's score depends on how many patients are meeting the requirements of the measure. For each measure, the provider earns a percentage first, which is then converted to a score out of 10 based on benchmarks (i.e. the better they perform against their peers, the higher their score per measure will be). The scores for the 6 measures are then put in a calculation to determine how many points the provider earns out of 30 for the Quality category.
ℹ️ NOTE
Practices who have 15 or fewer providers under a Tax ID Number will automatically earn 6 extra points towards their Quality numerator.
Cost (30%)
The Cost category measures Medicare spending per beneficiary and total per capita cost. The provider's score is automatically calculated from the billing codes that they submit via claims. Practices don’t need to complete any specific actions in Elation or submit anything in particular for this category. To optimize your scoring potential in this category, we recommend taking steps as a practice to minimize overall cost and hospitalizations for your patients.
Improvement Activities (15%)
For this category, CMS publishes a list of activities that are intended to improve care and outcomes. This is typically an easy category for practices to earn points. You can also learn more about Improvement Activities in our MIPS (2026) - Improvement Activities Category article.
For the 2026 MIPS performance year, scoring for the improvement activities categoryry has maintained some consistency to 2025 (when the category changed). Activities are not classified as high or medium-weight. To earn full credit in this performance category, you must simply meet the numerical requirement below that applies to your circumstances:
-
Clinicians, groups, and virtual groups with the small practice, rural, non-patient facing, or health professional shortage area special status must attest (submit a “yes”) to 1 activity.
-
All other clinicians, groups, and virtual groups must attest (submit a “yes”) to 2 activities.
Promoting Interoperability (25%)
This category requires 4 objectives, 2 registry integrations, a security audit, and a few attestations. Learn more about the Promoting Interoperability Performance Category in the MIPS (2026) - Promoting Interoperability Category article.
ℹ️ NOTE
Promoting Interoperability includes an automatic exception for small practices (i.e. 15 providers or fewer). The 25% will automatically be allocated towards the Quality and Improvement Activities measures.
A practice’s performance across the 4 MIPS categories (or fewer if reweighted) will result in a MIPS final score of 0 to 100 points.
This final score determines whether they will receive a negative (up to -9%), neutral, or positive (up to +9%) payment adjustment on their Medicare Part B Physician Fee Schedule payments in 2028.
To receive a neutral adjustment (i.e. avoid a penalty), practices who are required to participate in MIPS must earn at least 75 total points.
'Traditional MIPS' Participation Summary
After determining your MIPS eligibility and participation level, your practice can begin selecting and performing your measures and activities. To start, here is a timeline for each category:
| Quality | Cost | Improvement Activities | Promoting Interoperability |
|---|
| Clinicians must prioritize 6 measures, collecting data for each measure for the 12-month performance period (Jan 1 - Dec 31, 2026). | No action needed to collect or submit any data for cost measures. CMS calculates your Cost performance through your claims. | Clinicians must select between 1 to 2 activities, performing each activity for a continuous 90-day period in Calendar Year (CY) 2026. | Small practices (practices with 15 or fewer providers) are automatically excused from the PI category.
Clinicians who don't quality for this exclusion must collect data using CEHRT on the required measures for the same continuous 180- day performance period in CY 2026. |
*This table is only applicable to Traditional MIPS reporting. Reporting with an APM, or MVP will have different reporting requirements.
Tracking and Improvement During 2026
The QPP has multiple resources offered on their QPP resources site, through their help desk, and regularly updated on their newsletter.
*This article is provided for instructional purposes only. Elation Health does not support or guarantee anything other than relay useful information from various organizations. Elation Health also does not provide support for third-party technologies. We recommend consulting CMS guidelines for the most up to date information.
Copyright U.S Centers for Medicare & Medicaid Services. All rights reserved.
Resources
Related Articles



