Contents
Measure Details
Percentage of patients 18-85 years of age who had a diagnosis of essential hypertension starting before and continuing into, or starting during the first six months of the measurement period, and whose most recent blood pressure was adequately controlled (<140/90mmHg) during the measurement period
Measure Parameters
Patients whose blood pressure at the most recent visit is adequately controlled (systolic blood pressure < 140 mmHg and diastolic blood pressure < 90 mmHg) during the measurement period.
Patients 18-85 years of age who had a visit and diagnosis of essential hypertension starting before and continuing into, or starting during the first six months of the measurement period.
- Exclude patients with evidence of end stage renal disease (ESRD), dialysis or renal transplant before or during the measurement period.
- Exclude patients with a diagnosis of pregnancy during the measurement period.
- Exclude patients who are in hospice care for any part of the measurement period.
- Exclude patients receiving palliative care during the measurement period.
- Patients 66 and older by the end of the measurement period who are living long term a nursing home any time on or before the end of the measurement period.
- Exclude patients 66-80 with an indication of frailty for any part of the measurement period who meet any of the following criteria:
- Advanced illness diagnosis during the measurement period or the year prior
- OR taking dementia medications during the measurement period or the year prior
- Exclude patients 81 and older with an indication of frailty for any part of the measurement period.
Elation Workflows
ℹ️ NOTE
Elation has implemented dedicated workflows that reflect standardized requirements we do not control for certification to ensure structured and reportable tracking of measure specifications for supported electronic Clinical Quality Measures. To optimize performance per the specifications, please adhere precisely to the workflows outlined in the referenced Help Center article.
Patients must have an active diagnosis of hypertension recorded in their chart starting before and continuing into, or starting during the first six months of the measurement period. Elation looks for a hypertension ICD-10 code in either a visit note for the measurement period or in the Problem List.
To add a hypertension diagnosis to the Problem List:
| 1 | Go to the Problem List and click + Add Problem. |
| 2 | Search for the appropriate hypertension diagnosis and then select it from the results. |
| 3 | Adjust the Title and Dx Date as needed. |
| 4 | Click Save. |
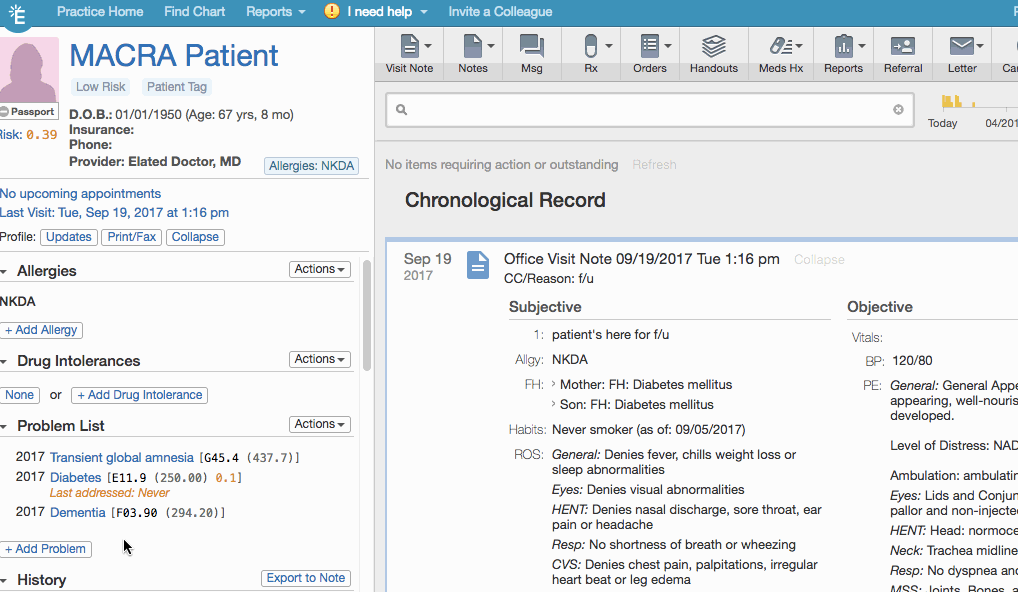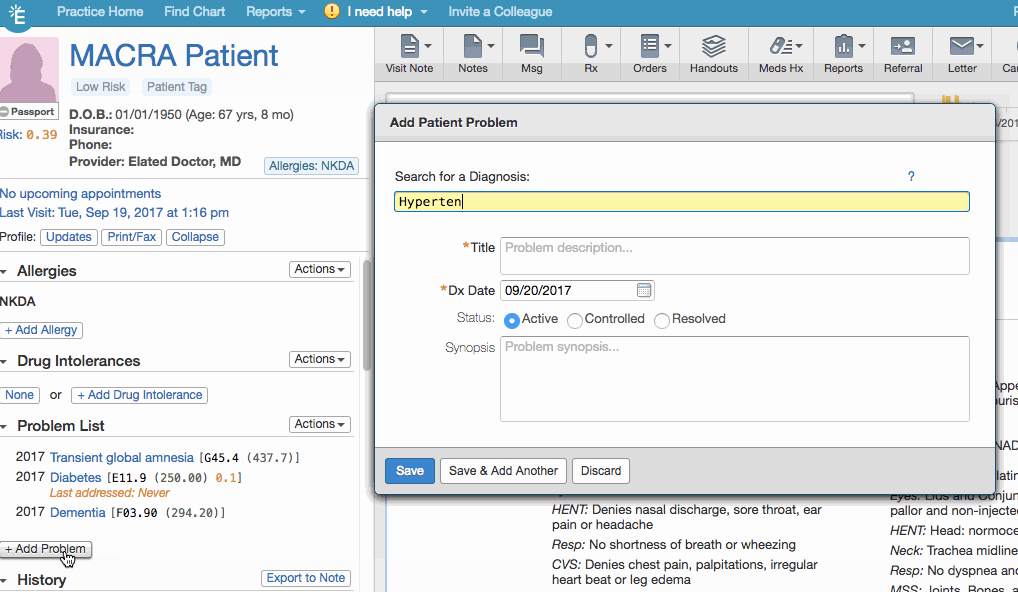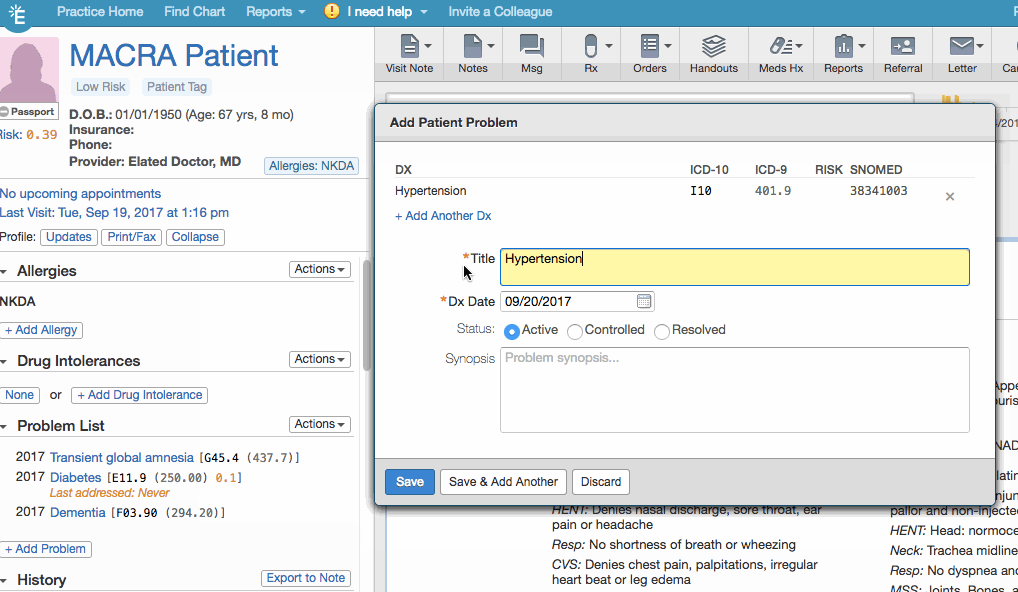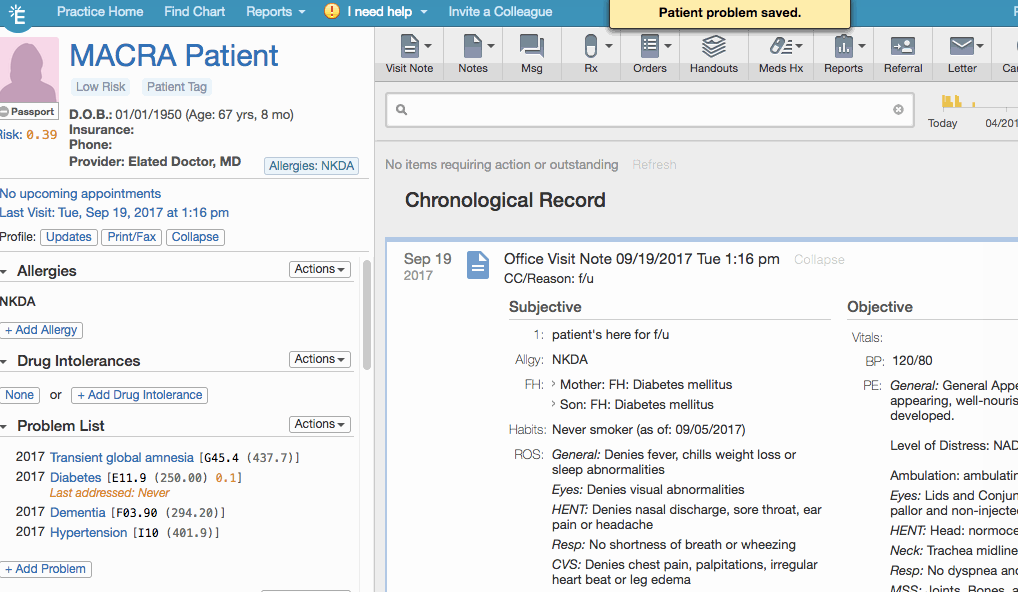
This workflow is applicable if ALL of the following denominator requirements are met:
| 1 | Record a blood pressure reading (both systolic and diastolic) in the Vitals section of the visit note. |
| 2a | If the blood pressure reading is within normal parameters (less than 140/90mmHg) then no further action is needed as the patient has met numerator requirements. |
| 2b |
If the blood pressure reading is outside of normal parameters (greater than 140/90mmHg) then:
- Click Address in the Blood pressure is not well controlled reminder at the top of the visit note draft.
- Choose from one of these 2 actions:
- Prescribe or modify medication
- Complete the prescription order as needed.
- Counsel patient on lifestyle changes (exercise, diet, stress, substance use)
- The text Counseled patient on lifestyle changes for hypertension will be appended to the visit note to indicate the patient met numerator requirements.
|
Clicking Dismiss will dismiss the reminder and the reminder will not appear again until a new visit note draft is opened.

| Exclusion/Exception | Steps |
|
Exclude patients with evidence of end stage renal disease (ESRD), dialysis or renal transplant before or during the measurement period.
|
- Click + Tag at the bottom of the visit note draft and add the appropriate document tag from this list:
- NEPHROPATHY: ESRD/PATIENT RECEIVED DIALYSIS
- NEPHROPATHY: KIDNEY TRANSPLANT STATUS
- PERITONEAL DIALYSIS PROCEDURE
- KIDNEY TRANSPLANT
-
Add a diagnosis of end stage renal disease (ESRD), dialysis or renal transplant in the patient’s Problem List or visit note with a start date on or prior to December 31, 2026.
|
|
Exclude patients with a diagnosis of pregnancy during the measurement period.
|
Add a diagnosis of pregnancy in the patient’s Problem List or visit note with a start date on or prior to December 31, 2026. |
|
Patients whose hospice care overlaps the measurement period.
|
Click + Tag at the bottom of the visit note draft and add the appropriate document tag from this list:
- EXCLUSION: HOSPICE CARE
- EXCLUSION: IP DISCHARGE STATUS TO HEALTH CARE FACILITY FOR HOSPICE CARE
- EXCLUSION: IP DISCHARGE STATUS TO HOME FOR HOSPICE CARE
|
| Patients receiving palliative care for any part of the measurement period. | Click + Tag at the bottom of the visit note draft and add the following document tag - EXCLUSION: PALLIATIVE CARE. |
| Patients 66 and older by the end of the measurement period who are living long term in a nursing home any time on or before the end of the measurement period. | Click + Tag at the bottom of the visit note draft and add the following document tag - EXCLUSION: Living Long Term in a Nursing Home. |
|
Exclude patients 66-80 with an indication of frailty for any part of the measurement period who meet any of the following criteria:
- Advanced illness diagnosis during the measurement period or the year prior
- OR taking dementia medications during the measurement period or the year prior
| See below. |
|
Exclude patients 81 and older with an indication of frailty for any part of the measurement period. | See below. |
Documenting frailty
To document frailty in Elation using
- Frailty diagnosis, advanced illness codes and/or medications
- Add a frailty diagnosis to the Problem List. You must select from one of the frailty codes listed here.
- Record one of the following:
- an advanced illness diagnosis in 2 outpatient encounters using one of the codes listed here.
- an advanced illness in 1 inpatient counter using one of the codes listed here.
- a dementia medication in the patient's chart.
- A frailty device code
- Click + Tag at the bottom of the visit note draft.
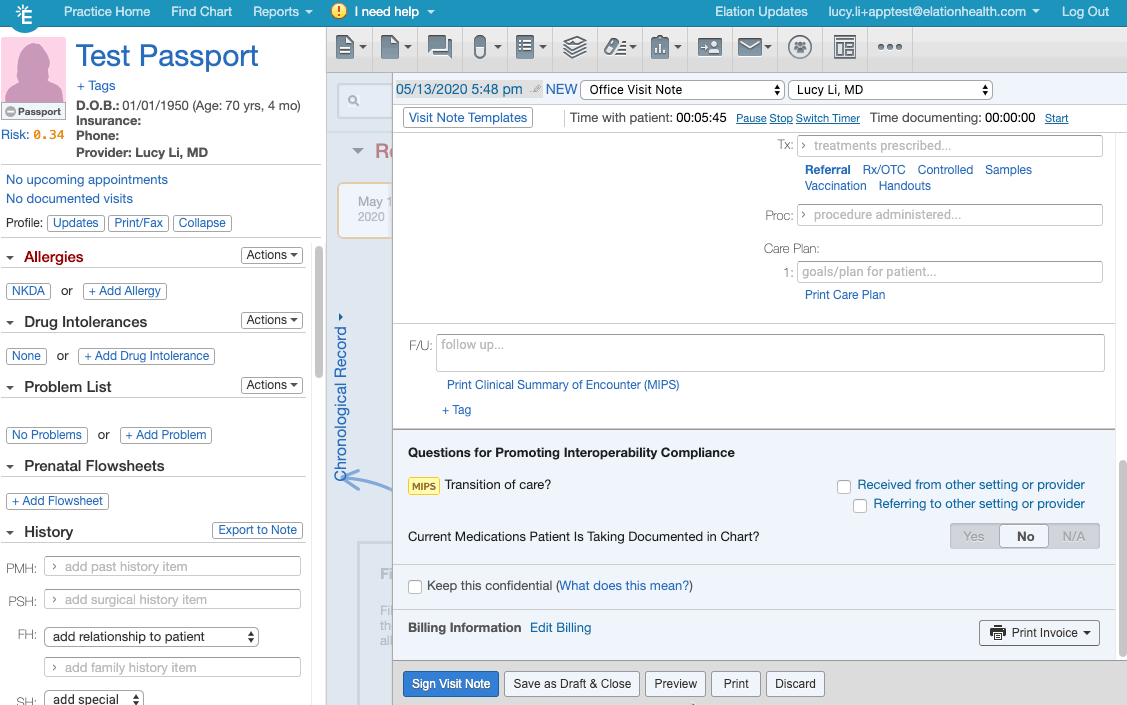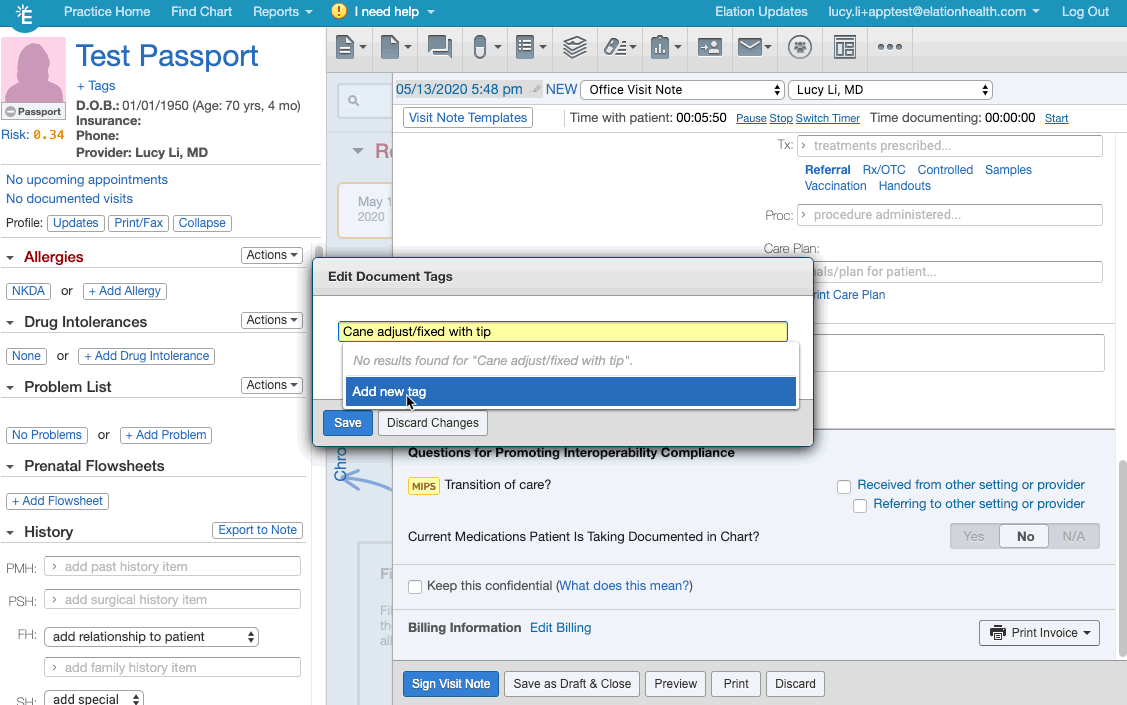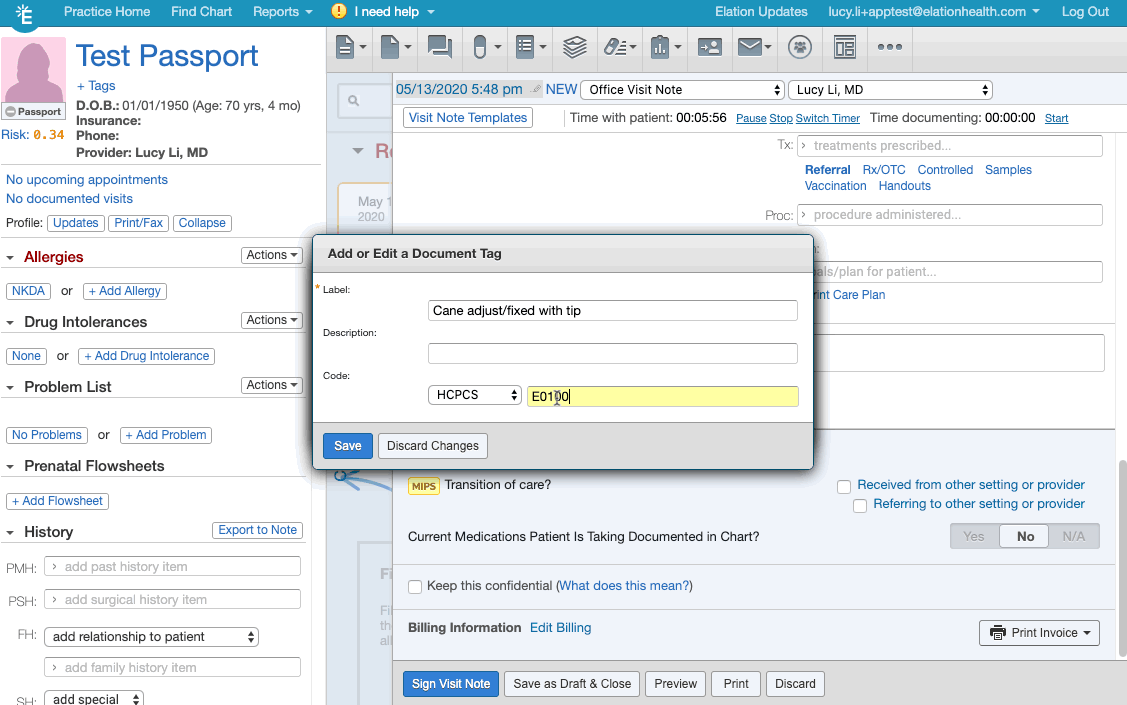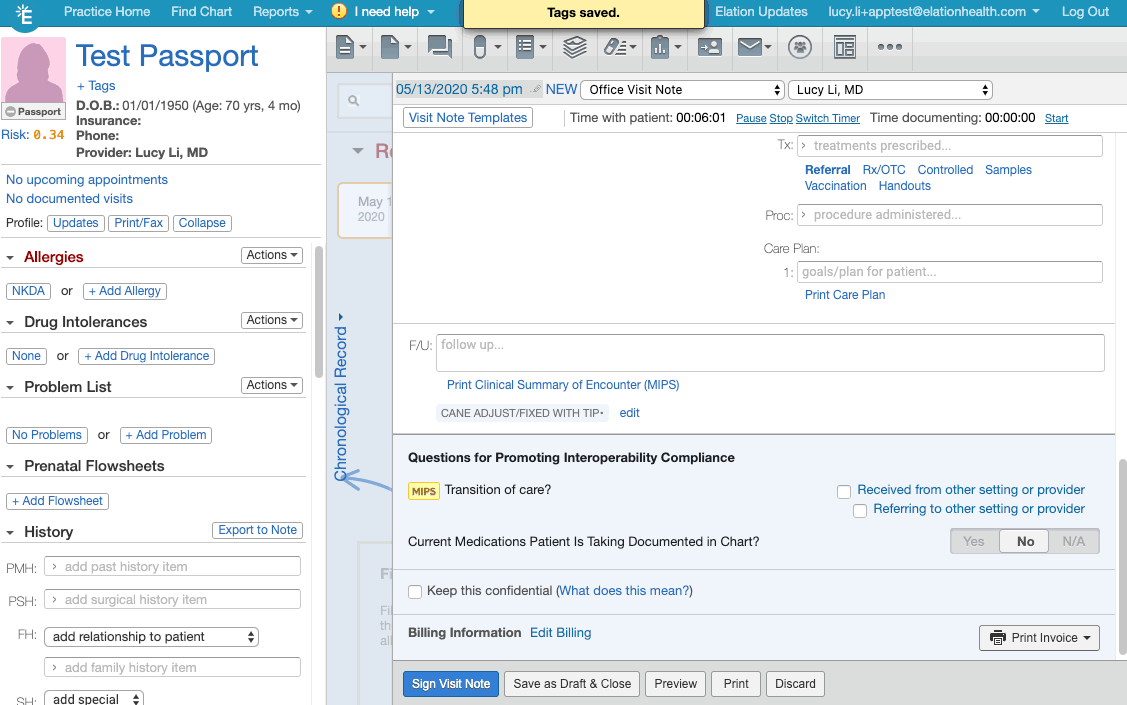
- Create/add the appropriate document tag for the relevant frailty device from this list of frailty device codes.
- If you are creating the document tag for the first time for a frailty device, make sure the document tag has the device's HCPCS code listed.
Measure Information
High blood pressure (HBP) or hypertension, known as the “silent killer,” increases risks of heart disease and stroke which are two of the leading causes of death in the U.S. (Yoon, Fryar, & Carroll, 2015). A person who has HBP is four times more likely to die from a stroke and three times more likely to die from heart disease (CDC, 2012). The National Vital Statistics Systems reported that in 2014 there were approximately 73,300 deaths directly due to HBP and 410,624 deaths with any mention of HBP (CDC, 2014). Between 2006 and 2016 the number of deaths due to HBP rose by 46.3 percent (Benjamin et al, 2019). Managing and treating HBP would reduce cardiovascular disease mortality for males and females by 30.4 percent and 38.0 percent, respectively (Patel et al., 2015).
The estimated annual average direct and indirect cost of HBP from 2014 to 2015 was $55.9 billion (Benjamin et al, 2019). Total direct costs of HBP is projected to increase to $220.9 billion by 2035 (Benjamin et al, 2019). A study on cost-effectiveness on treating hypertension found that controlling HBP in patients with cardiovascular disease and systolic blood pressures of >= 160 mm Hg could be effective and cost-saving (Moran, 2015).
Many studies have shown that controlling high blood pressure reduces cardiovascular events and mortality. The Systolic Blood Pressure Intervention Trial (SPRINT) investigated the impact of obtaining a SBP goal of <120 mm Hg compared to a SBP goal of <140 mm Hg among patients 50 and older with established cardiovascular disease and found that the patients with the former goal had reduced cardiovascular events and mortality (SPRINT Research Group et al., 2015).
Controlling HBP will significantly reduce the risks of cardiovascular disease mortality and lead to better health outcomes like reduction of heart attacks, stroke, and kidney disease (James et al., 2014). Thus, the relationship between the measure (control of hypertension) and the long-term clinical outcomes listed is well established.
Reference: Measure Information from CMS
Attachments
Related Articles



